12/4/19
The art of the possible….

Excitingly the Children and Young People’s Health Care Transformation #CYPHCT met for the first time this week as we begin to address how we can, together, across the country deliver the CYP elements of the NHS Long Term Plan https://www.england.nhs.uk/long-term-plan/
Sarah-Jane Marsh @BWCHBoss as magician in chief (or in @NHSEngland speak ‘the chair’) asked us to reflect on why we were there. For me it was a simple response, putting a focus on Child Health is what Children, Young People and families/carers have asked us to do, it’s what will help translate the wonderful work in the National Service Framework (2004) https://www.gov.uk/government/publications/national-service-framework-children-young-people-and-maternity-services, Children’s Outcomes Forum (2014) work https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/410482/CYPHOF_Report_2014-15.pdf along with contemporary evidence provided by the Royal College of Paediatrics and Child Health (RCPCH) https://www.rcpch.ac.uk/resources/state-child-health-england-two-years, amongst others that informed the CYP chapter in the NHS Longterm plan so that we can achieve better health outcomes for and with every child across the country, importantly focusing on those who are most vulnerable. Having a national ‘ask’ is a powerful driver for change at local, Sustainability and Transformation (STP)/Integrated Care System (ICS) levels and across regional patches.
The principles of voice/participation of the child/young person and families/carers not only in their care, but in the design and delivery of services are golden threads that strengthen with each iteration of how we progress the Child Health agenda, here are links to resources that have been developed over the years https://www.england.nhs.uk/participation/get-involved/how/forums/nhs-youth-forum/ Having Gabrielle of the NHS Youth Forum @NHSYouthForum at the table influencing the discussions is an important cultural shift, the transformation programme role modelled from the outset that working with children, young people and families who use services is the only way we can really make progress. The NHS Youth Forum response to the Long term plan demonstrates how passionately they want to be part of the work going forward in local health care systems as well as at a national level https://www.byc.org.uk/news/nhs-youth-forum-responds-to-nhs-long-term-plan
Perhaps if I’m honest the key thing that stood out for me from the conversation this week is that there isn’t a blueprint for this improvement work, we can only improve child health by all learning and sharing together, coaching and encouraging each other along the way, and so much great stuff is already happening. We’ve got a real opportunity to share the good stuff as the programme establishes, whether it’s getting children off tube feeds in Tower Hamlets and improving quality of life (along with making significant financial savings), ensuring that accessible information standards are being progressed in Sheffield to improve experiences and make best use of time with practitioners so that everyone’s time is valued, testing out the impact of youth workers in supporting young people with diabetes to reduce complications in later life or implementing the Child Bereavement experience measure (CBEM) to gain insight into the experiences of families when a child dies, there is so much Transformational work happening across the system.
Viv Bennett @VivJBennett and the team at Public Health England have done so much sustained work on the ‘Healthy Child Programme’ https://vivbennett.blog.gov.uk/tag/healthy-child-programme/ that offers a strong foundation as we step forward and onwards to truly transform child health outcomes across the whole system.
I’m excited by what’s ahead particularly as there’s a strong focus on the child health workforce and how we can ensure roles truly meet the evolving needs of child and families going forward, creative and courageous thinking is required!
So as #TeamChildHealth #CYPHCT moves forward, please do tweet, reflect on what matters most to you, share examples of brilliant stuff we need to spread, this programme will live and breath from the energy we all have to make a difference for and with the children and young people that we serve ….










 Day 2 took us from Charmouth back to Portland.
Day 2 took us from Charmouth back to Portland.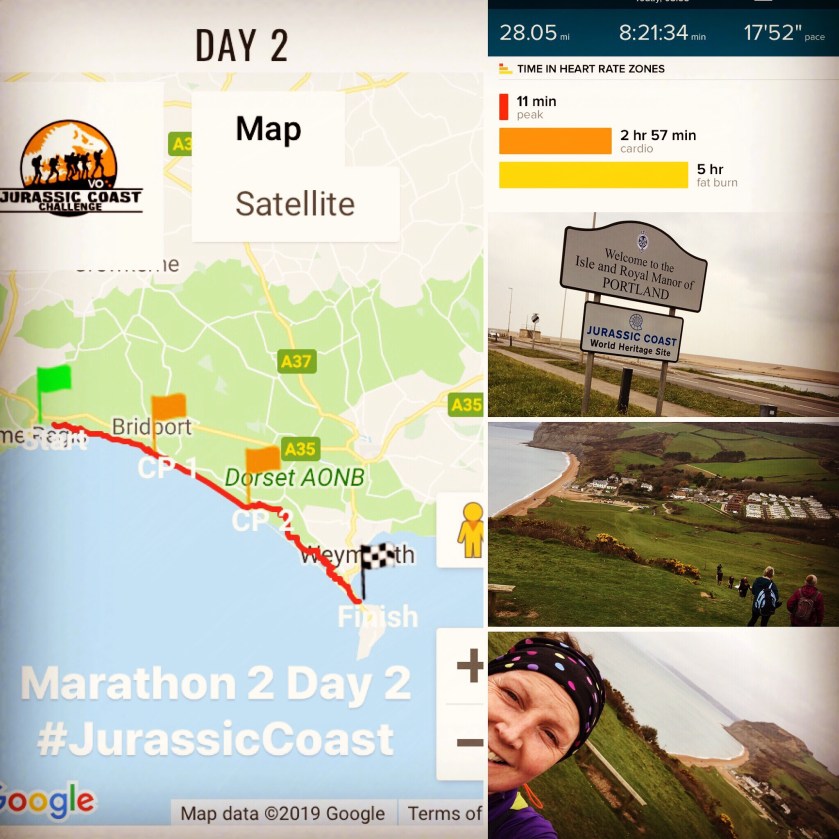





































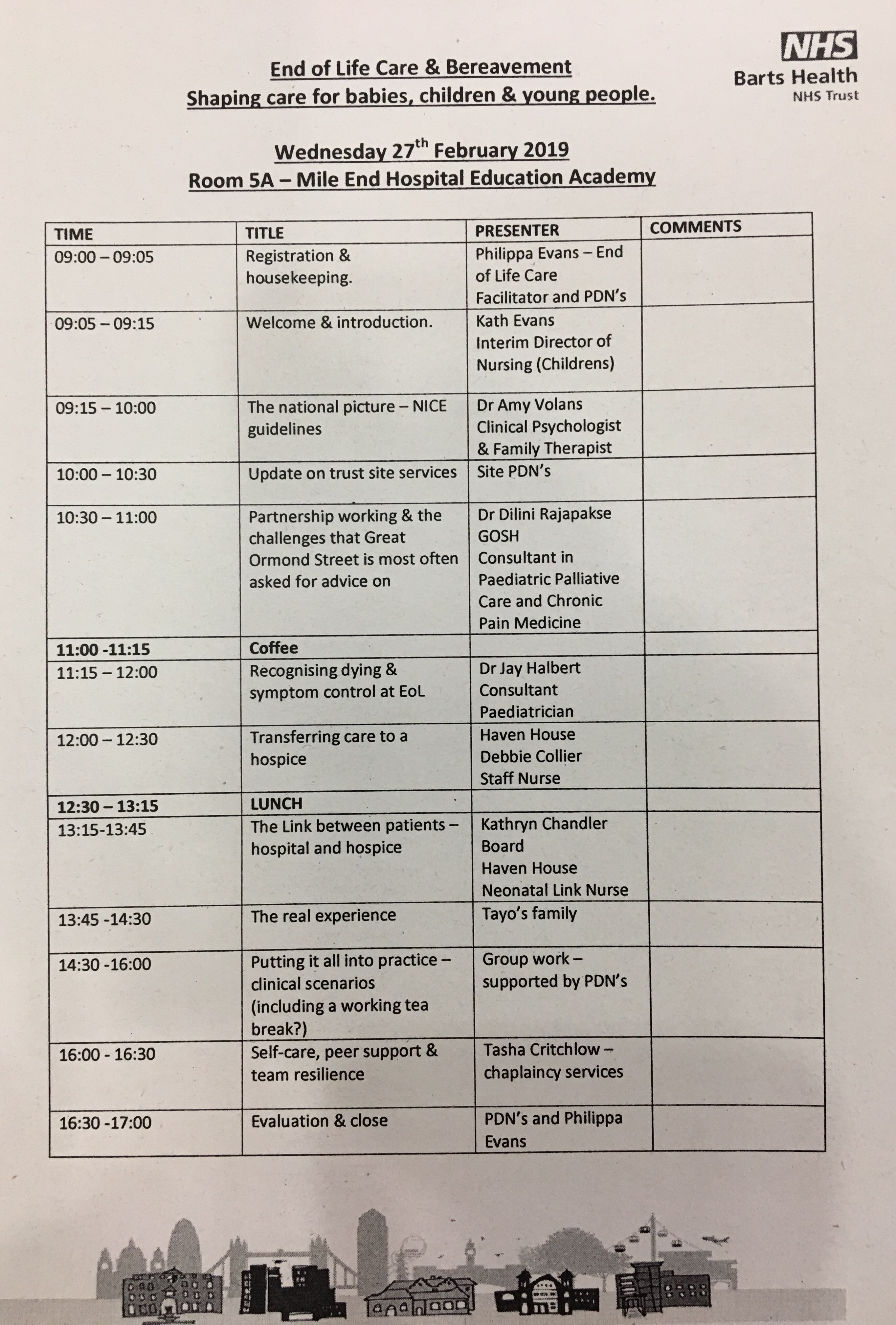












 Can social media help us grow professional curiosity? Here’s a link to some blogs on social media written with colleagues that may be of interest
Can social media help us grow professional curiosity? Here’s a link to some blogs on social media written with colleagues that may be of interest